For many, meat and dairy still feel like the cornerstone of a healthy meal. But growing evidence suggests there may be real health risks of animal protein worth paying attention to.
Foods like chicken, eggs, and cheese may not be as harmless as they seem. Studies are linking them to long-term health concerns that often fly under the radar.
In this post, we’ll look at 15 important health risks of animal protein—and why it might be time to take a closer look at what’s on your plate.
15 Health Risks of Animal Protein
1. IGF-1 from Animal Protein and Its Link to Cancer Risk
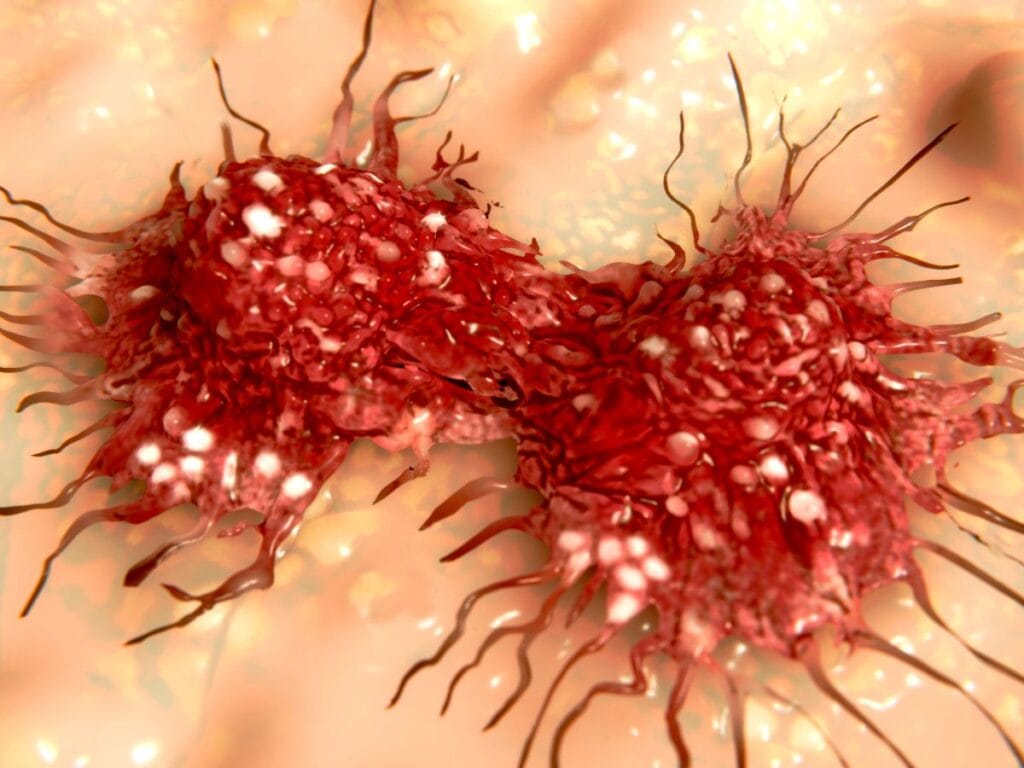
IGF-1 is your body’s growth accelerator hormone. Problem is, it can’t tell the difference between healthy cells and cancer cells. Both get the green light to multiply.
High animal protein intake cranks up your IGF-1 levels. Your liver starts pumping out more of this hormone when you’re constantly eating meat, dairy, and eggs. Those leftover hormones in animal products don’t help either.
Here’s what happens when you’re loading up on animal protein. Your liver goes into overdrive producing IGF-1. The residual hormones already in that steak give you an extra boost you don’t want. Your cellular growth pathways get stuck in the “on” position.
Studies show people eating tons of animal protein have higher IGF-1 levels. Higher IGF-1 means higher cancer risk for certain types. You’re basically giving potential cancer cells a growth hormone cocktail every time you sit down to a meat-heavy meal.
2. TMAO and Heart Disease: A Key Health Risk of Animal Protein
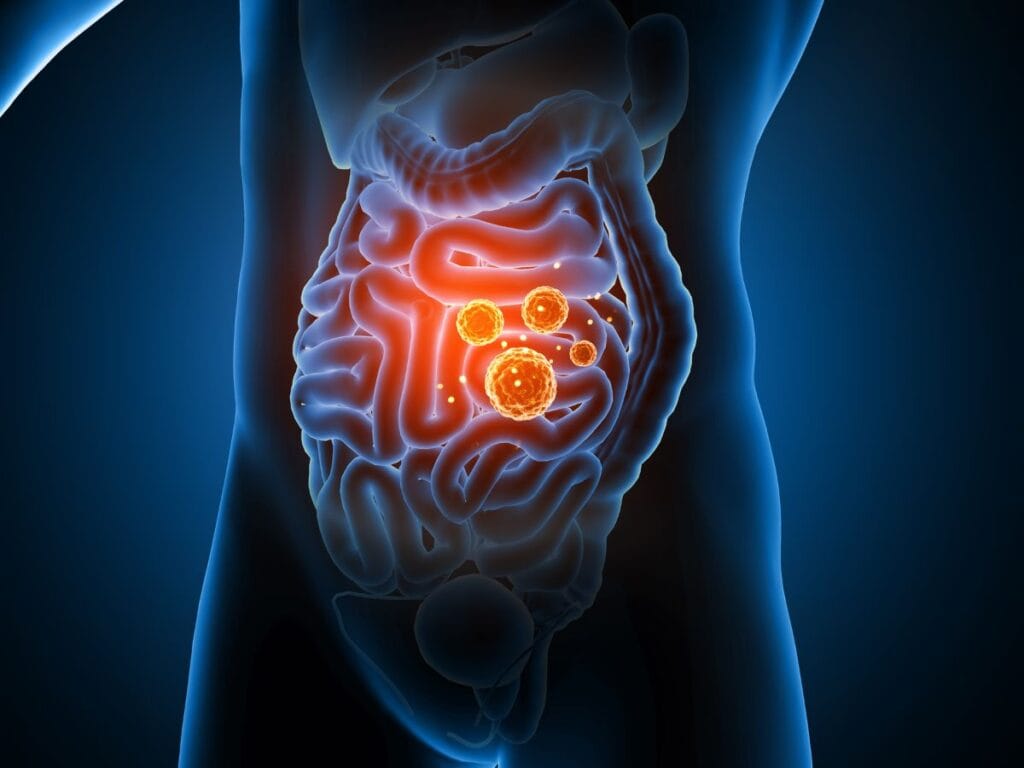
TMAO forms when you digest animal protein. Cleveland Clinic researchers found this compound can triple your risk of major heart problems. Your gut bacteria are basically creating a heart disease factory every time you eat meat.
Here’s the process that’s happening in your body. Your gut bacteria convert compounds in animal protein into trimethylamine (TMA). Your liver then converts TMA into TMAO, which builds up cholesterol in your artery walls.
More TMAO means more plaque and inflammation clogging your arteries. The New England Journal of Medicine published research showing higher TMAO levels significantly increase cardiovascular disease risk. You’re literally feeding the bacteria that create this dangerous compound.
Plant-based eaters make almost no TMAO, even when taking L-carnitine supplements. It’s not just the compounds in animal products causing problems. It’s the specific gut bacteria that flourish when you’re constantly eating meat, dairy, and eggs.
Switch to plant proteins and you avoid this whole mess. You get complete protein nutrition plus heart-healthy fiber and antioxidants. Your gut bacteria won’t be churning out TMAO to mess with your cardiovascular system.
3. The Lack of Antioxidants: An Overlooked Health Risk of Animal Protein
Think of oxidative stress as rust forming inside your body. Every time you eat animal proteins, especially red and processed meats, you’re speeding up that rusting process. Your cells are getting damaged while you’re just trying to hit your protein goals.
Cooking and digesting animal proteins creates free radicals. These cellular troublemakers damage your cells faster than your body can repair them. High animal protein intake overwhelms your natural defenses, creating oxidative stress.
It’s like having too many fires for your body’s firefighters to handle. Research shows this oxidative stress doesn’t just affect how you feel now. It speeds up aging from your skin to your organs.
Most people don’t realize their protein choices today determine how they’ll look and feel years down the line. That daily steak habit might be fast-tracking you to wrinkles and declining organ function. Meanwhile, plant proteins come packed with antioxidants that actually fight this damage.
Choose plant-based proteins and you get protection instead of oxidative stress. You’ll still hit your protein targets without accelerating the aging process. Your future self will thank you for not feeding your cells a steady diet of free radicals.
4. Heavy Metals in Animal Protein, Especially Seafood
Your favorite tuna sandwich comes with more than just protein. Heavy metals like mercury, cadmium, and lead accumulate in animal proteins, especially seafood. It’s like a toxic savings account you never opened.
Animals higher up the food chain collect these metals from their environment and prey. When you eat them, you’re getting concentrated doses of whatever pollutants they’ve been storing. Large predatory fish like tuna and swordfish are basically swimming mercury containers.
Land animals aren’t much better. They absorb cadmium and lead from contaminated soil and feed. These metals don’t just pass through your system—they stick around and potentially mess with your health over time.
Regular consumption means regular accumulation. Your body becomes the final stop in this toxic game of hot potato. Meanwhile, plant proteins don’t bioaccumulate heavy metals the same way.
You can avoid this whole mess by choosing plant-based proteins. No mercury, no cadmium buildup, just clean nutrition without the chemical baggage. Your kidneys and nervous system will appreciate not having to deal with a steady stream of heavy metals.
5. Health Risks of Dairy You Might Not Expect

The dairy industry calls milk nature’s perfect food. Reality check: conventional dairy contains hundreds of thousands of pus cells per milliliter from frequent udder infections. You’re basically drinking infected secretions with your cereal.
Those infections require constant antibiotics, contributing to antibiotic resistance. Modern dairy cows get milked while pregnant, pumping their milk full of estrogen and other hormones. Dairy products deliver 60-70% of the estrogen in a typical Western diet.
Excess estrogen exposure links to hormone-sensitive cancers and reproductive issues. Your daily latte habit might be messing with your hormonal balance more than you realize. Meanwhile, countries that guzzle the most dairy have the highest osteoporosis rates.
The calcium paradox is real: dairy’s high protein content actually increases calcium excretion through urine. You’re drinking milk for strong bones while potentially weakening them. About 65% of people are lactose intolerant anyway, suggesting our bodies aren’t designed for this stuff.
Dairy triggers inflammation in many people, contributing to acne, digestive problems, and autoimmune responses. Skip the pus-filled, hormone-loaded liquid meant for baby cows. Your body will thank you for not forcing it to process another species’ breast milk.
6. Heme Iron and the Health Risks of Animal Protein
Heme iron from animal proteins forces its way into your system whether you need it or not. Your body can’t regulate this absorption like it does with plant iron. You’re basically getting mandatory iron whether your stores are full or empty.
Excess heme iron acts like a free radical, triggering oxidative stress and inflammation throughout your body. This damages your kidneys and cardiovascular system over time. Studies link high heme iron intake to increased risks of type 2 diabetes, heart disease, and certain cancers.
Plant-based iron comes with built-in safety controls. Your body absorbs what it needs and ignores the rest, making iron overload nearly impossible. Plus, plant proteins package their iron with protective antioxidants and fiber.
Swapping animal protein for plant sources can slash heart disease risk by up to 30%. Too much animal protein overworks your kidneys, speeding up damage for those at risk of chronic kidney disease. Meanwhile, you’re forcing iron into a system that might already be overloaded.
Load up on kidney-friendly plant foods like quinoa, sweet potatoes, and leafy greens instead. You’ll get the iron you need without the oxidative damage. Your kidneys and heart will appreciate not being constantly assaulted by excess heme iron.
7. Cardiovascular Strain: A Major Health Risk of Animal Protein
Animal protein damages your heart beyond just saturated fat. Even lean meats independently contribute to heart disease development. A study tracking over 81,000 people found high animal protein consumers had 60% higher cardiovascular disease risk.
Animal protein creates an acidic environment in your body. To neutralize this acid load, your body pulls calcium from bones and deposits it in arterial walls, contributing to atherosclerosis. Most animal proteins also come loaded with sodium and inflammatory compounds that damage artery linings.
The good news? Swapping just 5% of your animal protein for plant protein can slash heart disease death risk by 25%. While red and processed meats raise cholesterol and clog arteries, plant proteins like lentils, chickpeas, and tofu deliver fiber, antioxidants, and potassium.
You’re basically choosing between foods that fuel your heart versus foods that attack it. Plant proteins come packaged with protective compounds instead of inflammatory ones. Your arteries won’t be constantly under assault from acidic byproducts and excess sodium.
Easy swap, healthier heart. Your cardiovascular system will appreciate not having to neutralize acid loads while dealing with arterial inflammation. Meanwhile, you’ll still hit your protein goals without the cardiac baggage.
8. Antibiotic Resistance and the Health Risks of Animal Protein

About 80% of antibiotics sold in the US go to livestock, not humans. Factory farms pump animals full of antibiotics to prevent disease in overcrowded conditions and promote faster growth. You’re eating the breeding ground for superbugs with your dinner.
The CDC reports antibiotic-resistant infections affect 2.8 million Americans annually, killing at least 35,000. Many of these resistant bacteria trace directly back to animal farming practices. Up to 81% of raw turkey, 55% of ground beef, and 39% of chicken samples contain antibiotic-resistant bacteria.
When you eat these animal products, those resistant bacteria can transfer their resistance genes to bacteria in your gut. Infections become difficult or impossible to treat, leading to longer hospital stays and increased mortality rates. The World Health Organization calls antibiotic resistance one of the top 10 global public health threats.
Your steak dinner might be contributing to the next superbug outbreak. These resistant bacteria don’t just disappear when you cook the meat. They’re setting up shop in your digestive system and sharing resistance genes with your existing gut bacteria.
Plant-based proteins eliminate this exposure entirely. Legumes, nuts, and whole grains don’t come with antibiotic-resistant bacteria attached. You’re protecting both your health and the effectiveness of life-saving antibiotics for future generations.
9. The Link Between Animal Protein and Type 2 Diabetes

Animal proteins contain specific amino acids like methionine and branched-chain amino acids (BCAAs) that directly interfere with insulin sensitivity. High levels of these amino acids trigger metabolic pathways that make your cells resistant to insulin. Your pancreas has to work overtime pumping out more insulin just to keep blood sugar stable.
Research shows people eating the most animal protein have significantly higher rates of type 2 diabetes compared to plant protein eaters. The amino acid profile in animal proteins activates mTOR pathways, which promote insulin resistance over time. It’s like reprogramming your cells to ignore insulin’s signals.
BCAAs from animal sources accumulate in your bloodstream and muscle tissue. This buildup interferes with glucose metabolism at the cellular level. Meanwhile, plant proteins contain different amino acid ratios that don’t trigger these problematic pathways.
Studies following thousands of people for decades show this isn’t about fat or cholesterol. It’s specifically about how animal protein amino acids mess with your body’s ability to process glucose. Even lean chicken and fish contribute to this effect.
Switch to plant proteins and you avoid this amino acid-induced insulin resistance. Your cells stay sensitive to insulin signals, keeping blood sugar stable naturally. No need to stress your pancreas with constant high insulin demands.
10. Animal Protein and Chronic Inflammation in the Body
Animal proteins contain arachidonic acid, an omega-6 fatty acid that your body converts into pro-inflammatory compounds called prostaglandins and leukotrienes. Plant proteins don’t contain arachidonic acid, so they can’t trigger this inflammatory cascade. You’re literally eating the building blocks for inflammation every time you choose animal over plant protein.
Neu5Gc is a sugar molecule found only in animal proteins that humans can’t naturally produce. When you eat it, your immune system creates antibodies against it, causing chronic inflammatory reactions. This immune response doesn’t happen with plant proteins because they don’t contain Neu5Gc.
Your gut bacteria also play a role here. Animal protein consumption shifts your microbiome toward pro-inflammatory bacterial strains that produce inflammatory metabolites. Meanwhile, plant protein feeds beneficial bacteria that produce anti-inflammatory short-chain fatty acids.
Research shows people eating high amounts of animal protein have elevated C-reactive protein levels, a key marker of systemic inflammation. This chronic inflammation contributes to everything from arthritis to autoimmune conditions. Your body is constantly fighting a low-level battle you probably don’t even realize is happening.
Switch to plant proteins and you remove these inflammatory triggers entirely. No arachidonic acid, no Neu5Gc, and a healthier gut microbiome that actually fights inflammation instead of promoting it. Your inflammatory markers drop and you’ll likely notice less joint pain and better energy levels.
11. Cancer Risk from Red and Processed Meat: A Known Health Risk of Animal Protein

The WHO classified processed meats like bacon, sausages, and ham as Group 1 carcinogens. That puts them in the same cancer-causing category as tobacco and asbestos. Your morning bacon habit is literally on par with smoking when it comes to cancer risk.
Nitrates and nitrites used as preservatives convert into N-nitroso compounds in your body. These compounds directly damage DNA and trigger tumor formation, especially in your colon. The smoking and curing processes create additional carcinogens like heterocyclic amines and polycyclic aromatic hydrocarbons.
High-temperature cooking methods like grilling create even more cancer-causing compounds. That charred steak you love is loaded with DNA-damaging chemicals. The American Institute for Cancer Research recommends avoiding processed meats entirely, not just limiting them.
Regular consumption increases your risk of colorectal cancer, type 2 diabetes, COPD, and cognitive decline. You’re basically eating a cocktail of known carcinogens every time you grab that deli sandwich. Meanwhile, plant-based alternatives like tempeh bacon offer similar textures without the cancer risk.
Skip the processed meat aisle entirely. Your DNA will thank you for not subjecting it to a daily dose of Group 1 carcinogens. There’s no safe amount of processed meat consumption according to cancer researchers.
12. Bone Loss: An Underestimated Health Risk of Animal Protein
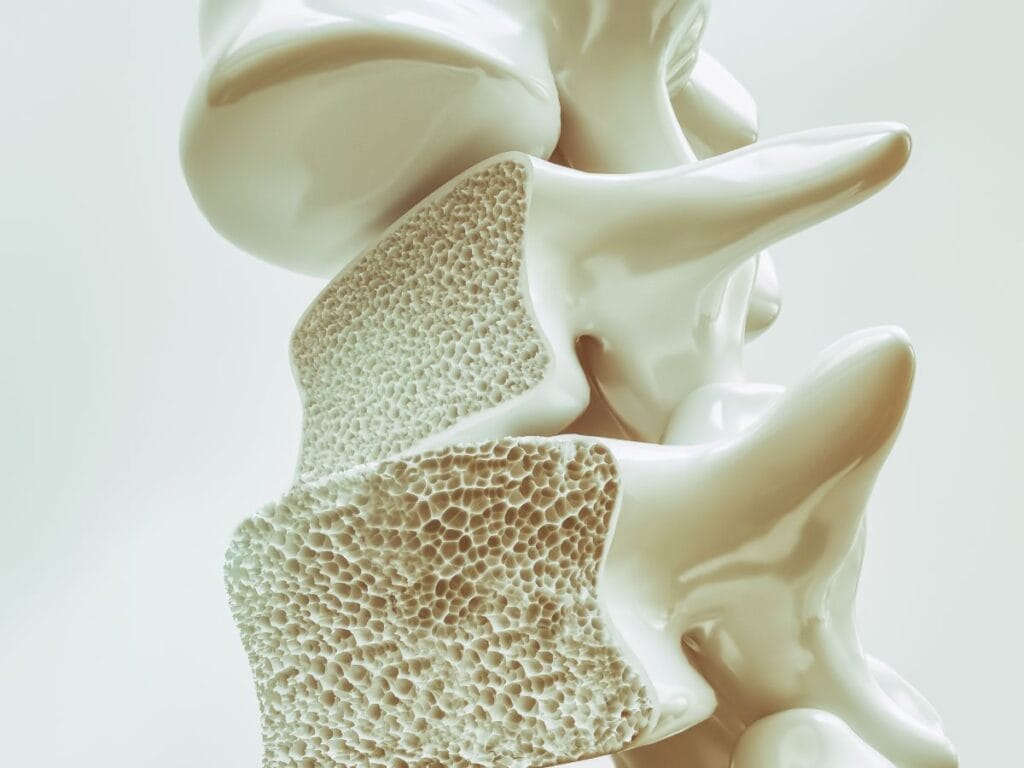
Animal protein creates an acidic load during digestion that forces your body to pull calcium from bones to neutralize the acid. For every gram of animal protein you eat, about 1.75 mg of calcium gets flushed out through your urine. Your skeleton becomes a calcium bank that gets constantly robbed to balance your blood pH.
This bone mineral buffering process happens automatically whenever you eat animal protein. Your body prioritizes maintaining proper pH over keeping calcium in your bones. Studies show higher animal protein intake correlates with increased calcium excretion and potentially higher fracture rates over time.
Countries with the highest dairy and meat consumption often have the highest osteoporosis rates. Meanwhile, populations eating primarily plant-based diets maintain stronger bones despite lower calcium intake. The acid-forming amino acids in animal proteins create a metabolic burden your bones have to pay for.
Plant proteins are either neutral or alkaline-forming during digestion. They don’t trigger the same calcium-leaching response that animal proteins do. Plus, plant foods come packaged with bone-supporting minerals like magnesium, potassium, and vitamin K.
Your daily protein choices are either supporting bone health or undermining it. Choose plant proteins and your bones won’t be constantly sacrificed to balance your body’s pH. Include calcium-rich foods like fortified plant milks, almonds, kale, and tahini for optimal bone support without the calcium drain.
13. Environmental Toxins: A Silent Health Risk of Animal Protein

Animals concentrate environmental pollutants in their tissues through bioaccumulation. Every toxin they encounter from contaminated feed, water, and air gets stored in their fat and organs. When you eat them, you’re getting a concentrated dose of whatever environmental nasties they’ve been collecting their entire lives.
Persistent organic pollutants (POPs) like dioxins, PCBs, and pesticides are fat-soluble chemicals that accumulate in animal fat. These compounds stick around in your body for years after exposure, potentially disrupting hormones and immune function. Fatty animal products deliver the highest concentrations of these toxic chemicals.
Factory farms often operate near industrial areas, exposing animals to additional contamination from air and water pollution. The animals become living pollution sponges, filtering environmental toxins into their meat, milk, and eggs. You’re essentially eating concentrated environmental contamination with every animal product.
Lead, cadmium, and arsenic also accumulate in animal tissues from contaminated feed and water sources. These heavy metals don’t just pass through animals—they build up over time and transfer directly to consumers. The higher up the food chain, the more concentrated these toxins become.
Plant foods don’t bioaccumulate environmental toxins the same way. They may absorb some pollutants from soil, but they don’t concentrate them through years of consuming contaminated feed. Skip the toxic middleman and go straight to plant proteins for cleaner nutrition.
14. Cognitive Decline: A Long-Term Health Risk of Animal Protein

Animal protein consumption correlates with faster cognitive decline in aging populations. Studies show people eating more processed and red meats have elevated markers of brain deterioration compared to plant protein eaters. Your daily protein choices might be affecting your future mental sharpness more than you realize.
The saturated fats in animal proteins can reduce blood flow to the brain by promoting atherosclerosis in cerebral arteries. Less blood flow means less oxygen and nutrients reaching brain tissue. Meanwhile, the cholesterol from animal products contributes to amyloid plaque formation, a hallmark of Alzheimer’s disease.
Animal proteins also lack the neuroprotective compounds found in plant foods. You’re missing out on brain-boosting antioxidants, flavonoids, and other compounds that support cognitive function. Plant proteins come packaged with nutrients that actually protect brain cells from damage.
Research following thousands of people for decades shows those eating the most animal protein have higher dementia risk. The amino acid profile in animal proteins may interfere with neurotransmitter production and brain metabolism. Your brain runs better on the nutrient profile that comes with plant proteins.
Switch to plant proteins and you get cognitive protection instead of potential harm. Foods like nuts, seeds, and legumes deliver brain-supporting nutrients along with their protein. Your future self will appreciate not having fed your brain a diet linked to cognitive decline.
15. Gut Health Disruption: One of the Many Health Risks of Animal Protein

Animal protein fermentation in your gut produces toxic byproducts like hydrogen sulfide and p-cresol. These compounds directly damage your intestinal lining and trigger chronic inflammation. Your gut bacteria literally turn animal protein into poison that irritates your digestive system from the inside.
High animal protein intake also reduces beneficial bacterial diversity in your microbiome. You end up with an overgrowth of putrefactive bacteria that thrive on protein while crowding out helpful strains. This bacterial imbalance weakens your immune system and affects everything from mood to nutrient absorption.
The saturated fats in animal products increase intestinal permeability, creating “leaky gut syndrome.” Harmful substances leak through your damaged gut barrier into your bloodstream, triggering systemic inflammation and potentially contributing to autoimmune conditions. Your intestinal wall becomes a sieve instead of a protective barrier.
Plant proteins feed beneficial bacteria that produce protective short-chain fatty acids. These compounds actually heal and strengthen your gut lining instead of damaging it. You get diverse, healthy gut bacteria that support immune function and overall health.
Skip the gut-damaging animal proteins and choose plant alternatives that nourish your microbiome. Your digestive system will thank you for not feeding it a steady diet of inflammation-causing byproducts. A healthy gut means better immunity, mood, and nutrient absorption.
Conclusion: Making Conscious Choices
Look, the evidence is pretty clear: animal protein comes with a laundry list of health risks you probably never thought about. From IGF-1 cranking up cancer growth to TMAO wreaking havoc on your heart, you’re getting way more than just protein with that steak dinner. Your gut bacteria are producing toxins, your bones are getting robbed of calcium, and your brain might be paying the price down the road.
Don’t panic and throw out everything in your fridge tonight. But maybe start questioning whether that daily bacon habit is worth the Group 1 carcinogen classification. Or if those antibiotic-resistant bacteria in your chicken are really what you want colonizing your gut.
Plant proteins deliver the same muscle-building benefits without the toxic baggage. No heavy metals, no inflammatory compounds, no cancer-causing preservatives. Just clean protein that comes packaged with fiber, antioxidants, and nutrients that actually protect your health instead of undermining it.
You don’t have to go full vegan overnight and survive on sad lettuce leaves. Start small—swap one meat meal for lentils this week. Try tempeh bacon instead of the real thing. Your future self will thank you for not feeding your body a steady stream of compounds linked to heart disease, cancer, and cognitive decline.
The choice is yours: keep eating concentrated environmental toxins and inflammation triggers, or switch to proteins that actually support your long-term health. Your kidneys, heart, gut, and brain are all waiting to see what you decide.
References
- Food and Agriculture Organization of the United Nations (FAO)
“Livestock’s Long Shadow: Environmental Issues and Options.”
URL: http://www.fao.org/3/a0701e/a0701e.pdf - World Health Organization (WHO)
“Healthy Diet: Fact Sheet.”
URL: https://www.who.int/news-room/fact-sheets/detail/healthy-diet - National Institutes of Health (NIH)
“Red Meat Consumption and Health Outcomes.”
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5562601/ - Environmental Working Group (EWG)
“Meat Eater’s Guide to Climate Change + Health.”
URL: https://www.ewg.org/meateatersguide/ - ScienceDirect
“Water Use and Efficiency in Livestock Production Systems.”
URL: https://www.sciencedirect.com/ - United Nations Environment Programme (UNEP)
“Food Waste Index Report 2021.”
URL: https://www.unep.org/resources/report/unep-food-waste-index-report-2021 - The Lancet Planetary Health
“The Environmental Impacts of Dietary Choices.”
URL: https://www.thelancet.com/planetary-health - Our World in Data
“Environmental Impacts of Food Production.”
URL: https://ourworldindata.org/environmental-impacts-of-food

